Noninvasive Vascular Laboratory
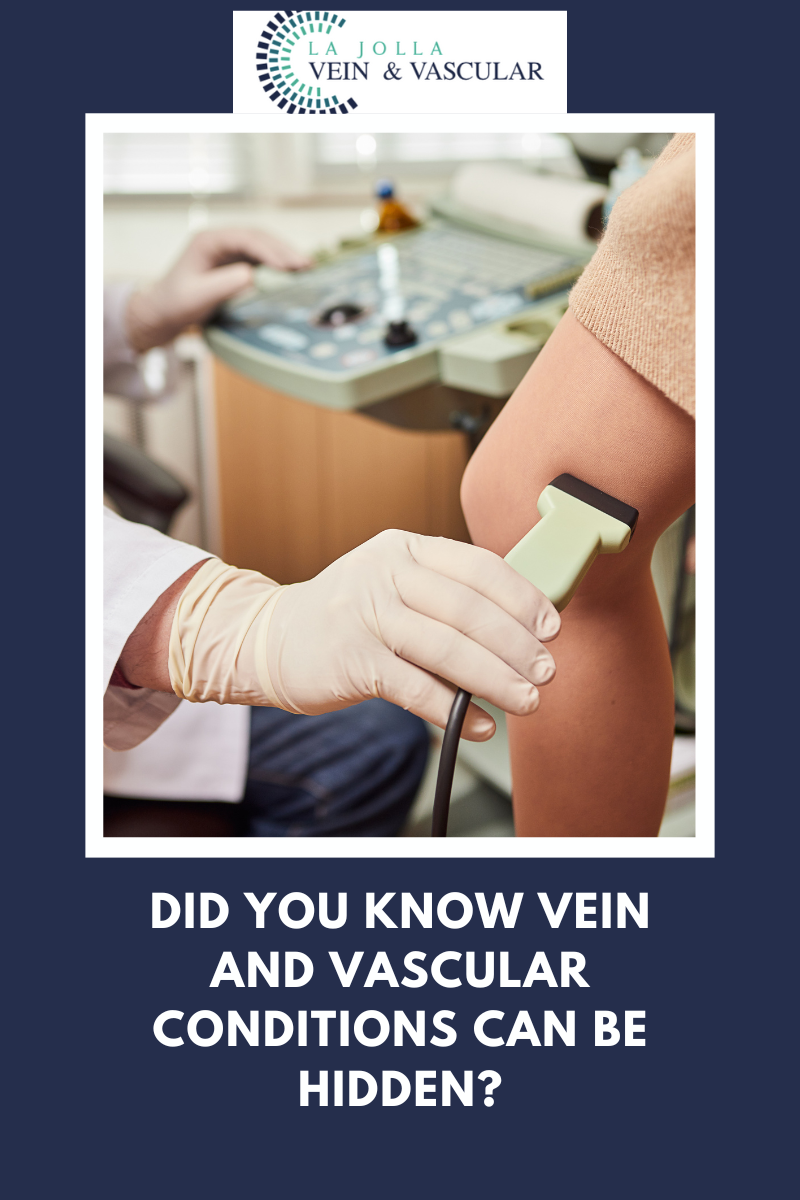
The Vascular Laboratory at La Jolla Vein & Vascular utilizes advanced, noninvasive, diagnostic, medical ultrasound technology while ensuring high quality results to detect diseases that may affect blood flow in the arteries and veins. We utilize “state-of-the-art” color duplex ultrasound imagers and indirect testing equipment.
The Vascular Lab offers the convenience of:
- Non-invasive testing
- Same-day imaging appointments
- Follow-up clinic visits with our on-site vascular team
- Appointments at multiple locations including La Jolla, Poway, Chula Vista, and Solana Beach.
What is Duplex Ultrasound
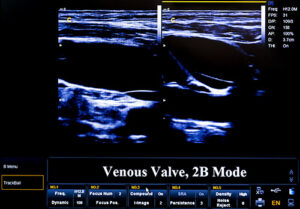
Duplex ultrasound involves using high frequency sound waves to look at the speed of blood flow, and structure of the blood vessels. The term “duplex” refers to the fact that two modes of ultrasound are used, Doppler and B-mode. The B-mode transducer obtains an image of the vessel being studied. The Doppler probe within the transducer evaluates the velocity and direction of blood flow in the vessel.
Types of Ultrasound Testing Offered:
Direct testing (duplex imaging)
Venous
- Deep Vein Thrombosis- upper or lower extremity
- Venous Reflux
Arterial
- Abdominal Aorta
- Abdominal Aortic Aneurysm (AAA) Screening- must meet criteria of SAAAVE Act
- Carotid Duplex
- Lower Extremity Duplex
Indirect testing (non-imaging)
- Arterial –Ankle Brachial Index (ABI) with waveforms
- Arterial -Segmental pressures and waveforms (P&Ws), upper or lower extremity
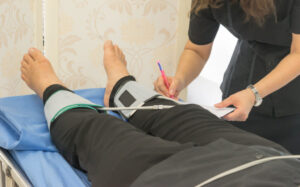
Check pulse measurement of vascular examination
Who Performs the test?
Accuracy is critical. Our ultrasounds are ALWAYS performed by a credentialed sonographer, called a Registered Vascular Technologist (RVT). An RVT is a sonographer who completed a two-year ultrasound program, plus additional clinical training and obtained certification by meeting the highest standards by The American Registry for Diagnostic Medical Sonography® (ARDMS®). It is important that a specially trained RVT perform the study, because a special protocol must be followed for each study to meet accreditation standards. The protocol involves taking images at certain anatomic locations using special waveforms to show blood flow. All images taken by the RVT are reviewed by the physician.
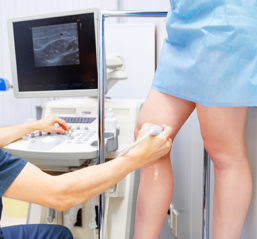
Learn More About Testing
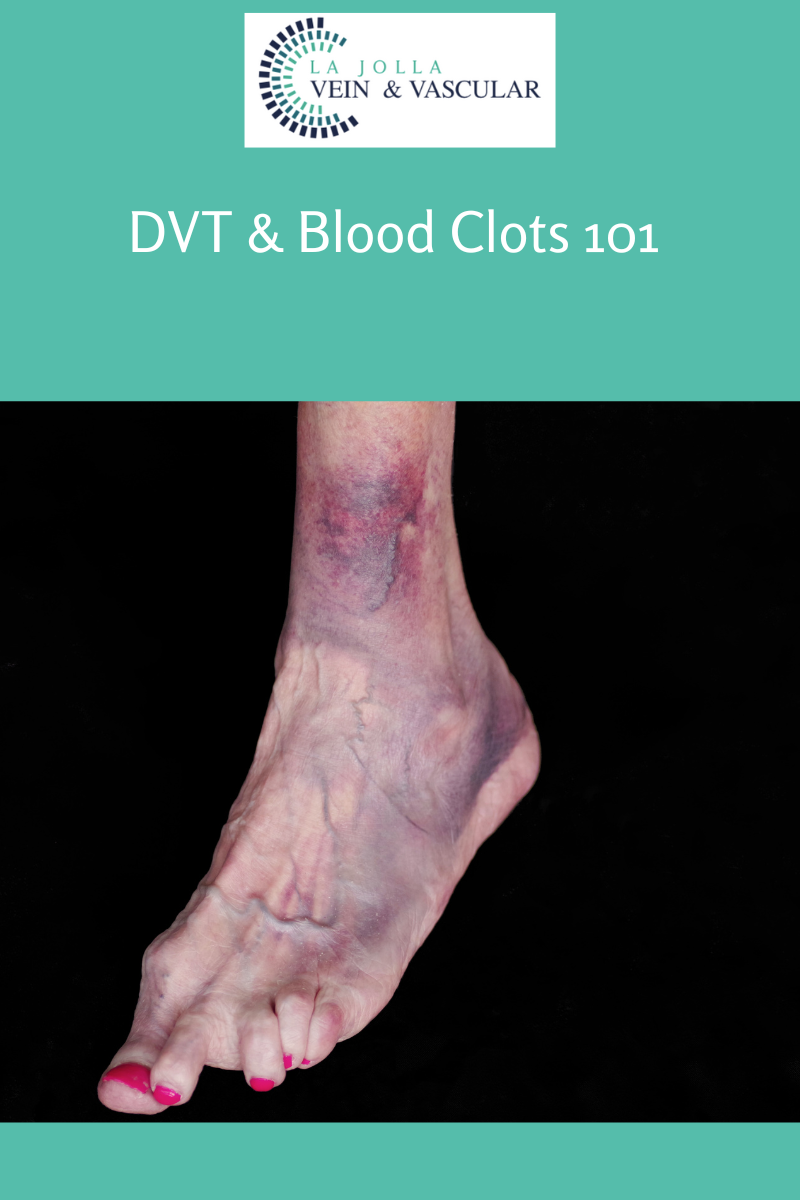
Deep Vein Thrombosis (DVT) Ultrasound
Venous ultrasound uses sound waves to produce images of the veins in the body. It is commonly used to search for blood clots, especially in the veins of the leg – a condition often referred to as deep vein thrombosis. Ultrasound does not use ionizing radiation and has no known harmful effects.
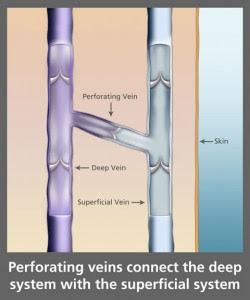
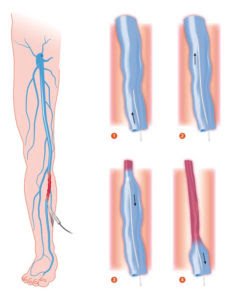
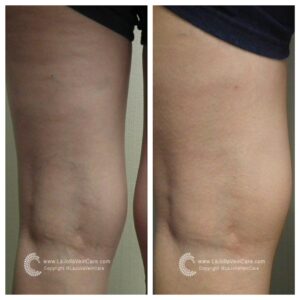
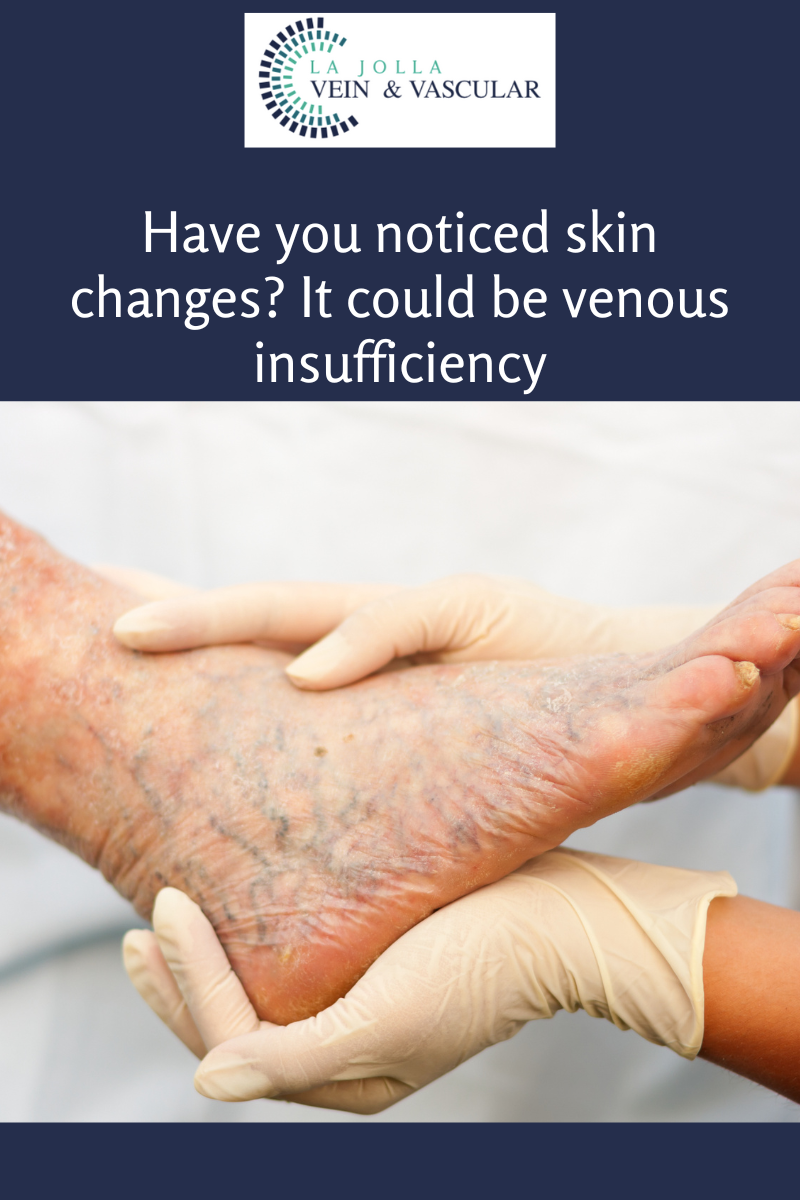
Venous Reflux Ultrasound
Ultrasound looks at deep and superficial veins in the legs to check for venous-valvular incompetence (the underlying condition that causes varicose veins). The ultrasound examination is used to both identify the veins that have faulty valves and to map the anatomy of the veins, creating a ‘road map.’ This is necessary to make an accurate assessment of the cause and extent of the varicose veins, as well as to formulate the best treatment plan. This should be done for any individual being evaluated for varicose veins, leg swelling, skin changes, patients who have failed prior treatment, patients who are symptomatic and in some patients with certain anatomic patterns of spider veins. Up to 40 million Americans have varicose veins. Left untreated, the veins may become worse.
Before your test:
This study does not require any preparation. You should not wear your compression stockings the same day as the examination. Make sure to be hydrated.
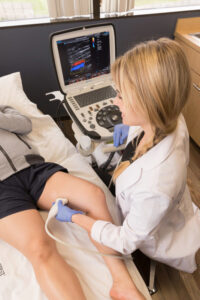
Carotid Artery Ultrasound
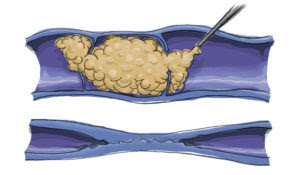
Ultrasound evaluation of the carotid arteries that screens for buildup of fatty plaque — one of the leading causes of strokes. Carotid arteries are the main blood vessels to the brain. They can develop a buildup of plaque caused by atherosclerosis, or hardening of the arteries. When the buildup becomes very severe, it can cause a stroke. A stroke occurs when part of the brain is damaged by these vascular problems; in fact, 80 percent of strokes are “ischemic strokes” where part of the circulation to the brain is cut off, usually due to blockages in the carotid arteries. The process is similar to the buildup of plaque in arteries in the heart that causes heart attacks. Strokes are the third leading cause of death in the United States according to the National Center for Health Statistics.
Peripheral Arterial Disease Testing
This test uses ultrasound and blood pressure measurements to check for peripheral arterial disease (plaque build-up) in the lower extremities. If you get leg cramps when you walk, it may be a sign of PAD. Learn more about keeping your legs healthy. Peripheral arterial disease (PAD) occurs when atherosclerosis, or hardening of the arteries, causes a buildup of plaque in the blood vessels that carry oxygen and nutrients to all the tissues of the body. As these plaques worsen, they reduce essential blood flow to the limbs and can even cause complete blockages of the arteries. Early on, PAD may only cause difficulty walking, but in its most severe forms, it can cause painful foot ulcers, infections, and even gangrene, which could require amputation. People with PAD are three times more likely to die of heart attacks or strokes than those without PAD.
Abdominal Aortic Aneurysm
The abdominal aorta serves the entire lower half of the body.
Abdominal Aortic Aneurysm (AAA) is an enlargement or “bulge” that develops in a weakened area within the largest artery in the abdomen. The pressure generated by each heartbeat pushes against the weakened aortic wall, causing the aneurysm to enlarge. If the AAA remains undetected, the aortic wall continues to weaken, and the aneurysm continues to grow. Eventually, the aneurysm becomes so large, and its wall so weak, that rupture occurs. When this happens there is massive internal bleeding, a situation that is usually fatal. The only way to break this cycle is to find the AAA before it ruptures. Nearly 200,000 people in the U.S. each year are diagnosed with an AAA, which can be deadly without treatment
“Bringing Experts Together for Unparalleled Vein and Vascular Care”
La Jolla Vein & Vascular (formerly La Jolla Vein Care) is committed to bringing experts together for unparalleled vein and vascular care.
Nisha Bunke, MD, Sarah Lucas, MD, and Elliot DeYoung, MD are specialists who combine their experience and expertise to offer world-class vascular care.
Our accredited center is also a nationally known teaching site and center of excellence.
For more information on treatments and to book a consultation, please give our office a call at 858-550-0330.
For a deeper dive into vein and vascular care, please check out our Youtube Channel at this link, and our website https://ljvascular.com
For more information on varicose veins and eliminating underlying venous insufficiency,
Please follow our social media Instagram Profile and Tik Tok Profile for more fun videos and educational information.
For more blogs and educational content, please check out our clinic’s blog posts!