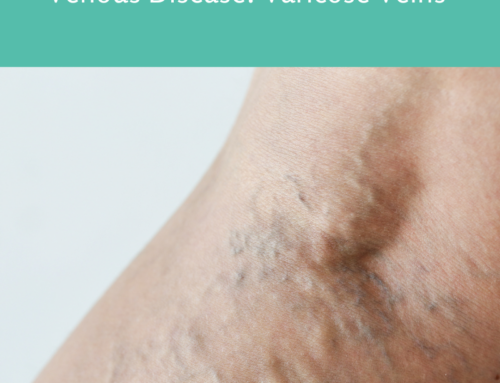
Changing Insurance Requirements for Varicose Vein Treatment
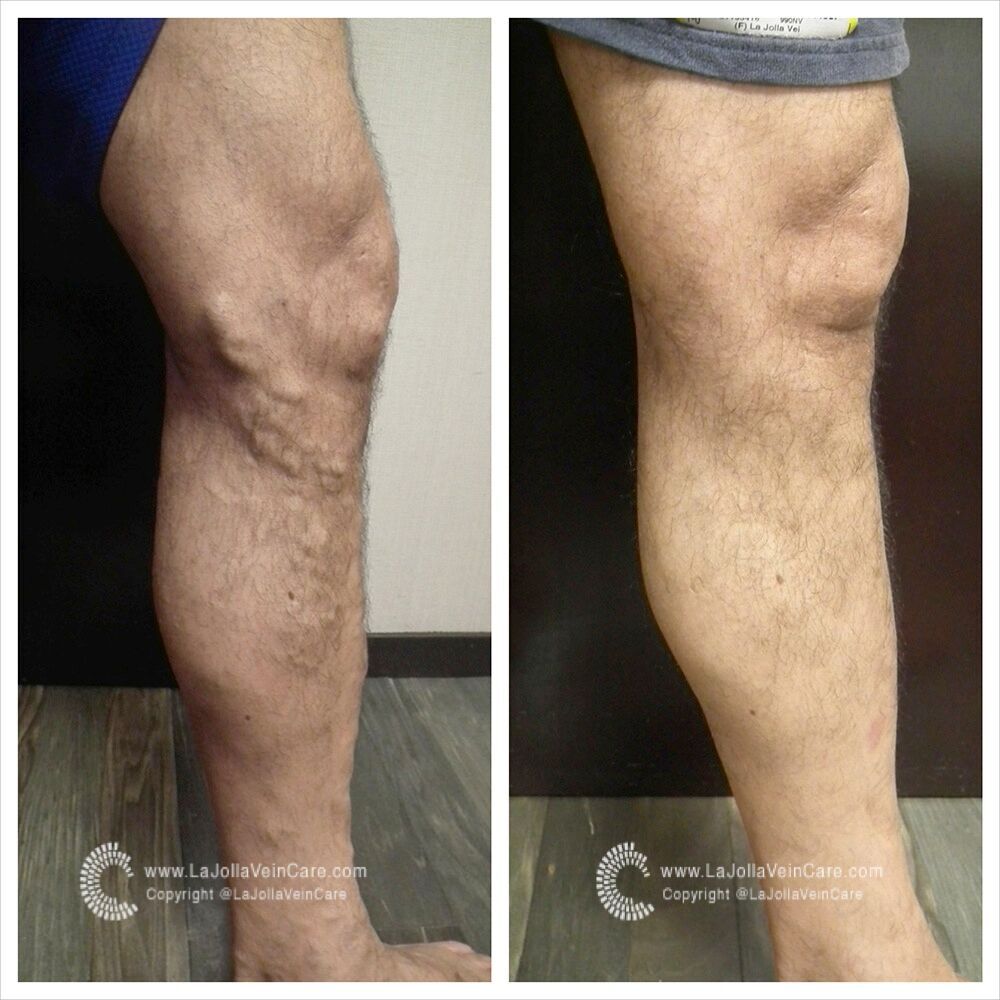
Compression stockings and socks are an important part of the regimen for the treatment of varicose veins. Insurance will require that they are used for 6-12 weeks prior to approving and paying for varicose vein treatment. The good news is that compression socks and stockings are available now in a wide variety of fashion styles and colors. Because new styles of compression socks are more fashion-friendly, you can integrate medical therapy into your wardrobe for work and casual attire. Fashion compression can be found at compressrx.com.
We have noticed a trend over the past year regarding insurance coverage for varicose veins; Insurance is increasingly becoming stricter with its policies for varicose vein coverage. Insurance policies vary from person to person regarding whether or not their policy will cover the actual vein treatment (office visits, diagnostic ultrasound examinations, and consultations are typically covered benefits by most). Most insurance types now require that an individual has worn and tried medical-grade compression for over 3 months before they can be considered for varicose vein treatment. Specifically, the patient has to have been using medical-grade compression for 3-months or longer and still has not had improvement in symptoms. The exceptions are Medicare and Anthem require only a six-week trial of compression. Compression socks and stockings are part of conservative management for vein conditions. Medical grade compression socks are stronger than over-the-counter socks and may require a prescription. Because your insurance may require 3 months of wearing compression socks/stockings before they will pay for your medical vein procedure, you should start wearing them as soon as possible and document it. For example, ask your primary care physician for a prescription. Keep your receipts for the purchase, as sometimes insurance requires proof of when you started using compression. Insurance usually does not cover compression stockings but a flexible health savings account can typically be used. Compression stockings should be used as a trial of conservative treatment in addition to leg elevation, exercise, weight loss, and NSAIDs. We are happy to answer questions about insurance coverage for vein procedures. Please call us at 858-550-0330.