Deep Vein Thrombosis (DVT): Understanding the Silent Threat to Vascular Health
LJVascular2023-10-11T16:50:51-07:00Deep Vein Thrombosis (DVT): Understanding the Silent Threat to Vascular Health
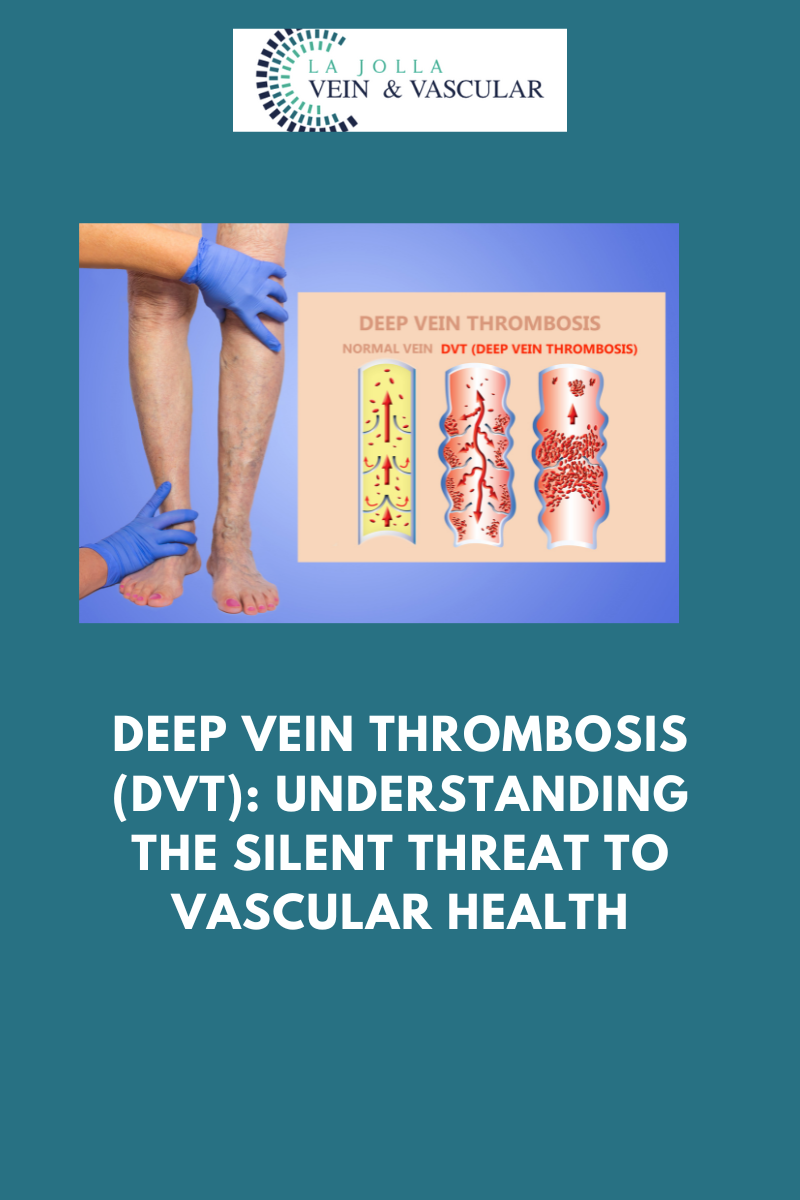
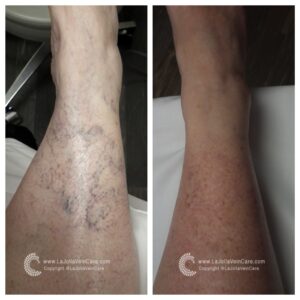
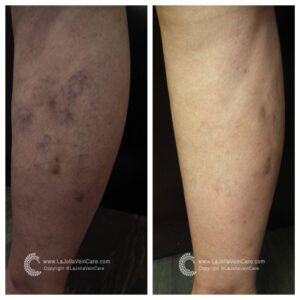
Deep Vein Thrombosis, more commonly known as DVT, is a medical condition characterized by the formation of blood clots deep within the veins of the lower extremities. While these clots may remain concealed beneath the surface, the lurking danger they represent should never be underestimated. In this blog post, we embark on an in-depth exploration of DVT, unraveling its intricacies, recognizing the severity of this medical condition, elucidating the diagnostic process, and emphasizing the paramount importance of staying vigilant in its detection.
Deciphering Deep Vein Thrombosis (DVT)
Deep Vein Thrombosis, the ominous acronym of DVT, is a condition where blood clots form within the deep veins of the legs. The initial appearance of these clots might deceive, seemingly harmless; however, the true peril emerges when they venture into the bloodstream. If these clots journey to the lungs, they can give rise to a potentially life-threatening condition known as a pulmonary embolism.
The Pivotal Role of Duplex Ultrasound in Diagnosis
Diagnosing DVT stands as a pivotal stride towards averting its perilous consequences. This is where Duplex ultrasound, a priceless diagnostic instrument, assumes its critical role. Here is an insight into its functionality:
Experienced Vascular Sonographer: A proficient vascular sonographer serves as the linchpin in the diagnosis of DVT. Their expertise is the bedrock upon which accurate and reliable results are founded.
Duplex Ultrasound Examination: Duplex ultrasound amalgamates the prowess of traditional ultrasound, denoted as B-mode, with Doppler ultrasound. This fusion empowers healthcare providers to visualize the flow of blood and identify clots within the deep veins.
Indications for DVT Study: A DVT study is typically conducted when an individual presents with discernible signs and symptoms of lower extremity DVT. These symptoms often encompass leg pain and swelling, frequently accompanied by telltale signs like redness and warmth.
Routine Screening: In specific circumstances, such as post-vein procedures or other surgical interventions, routine DVT screening may be undertaken as a precautionary measure to identify clots before they manifest harm.
Preparation for the DVT Study
Fortunately, preparing for a DVT study is a straightforward endeavor, devoid of intricate steps. Here are the salient points to keep in mind:
No Special Preparation: In contrast to certain medical tests that mandate fasting or adherence to specific preparations, a DVT study typically necessitates no extraordinary measures.
Vigilance Beyond the Lower Limbs: The Upper Extremity Venous Study
Although DVT is conventionally associated with the lower extremities, it is imperative to recognize that blood clots can potentially take root elsewhere within the body. This includes the upper arms and neck. An Upper Extremity Venous Study is a diagnostic ultrasound procedure designed to investigate the upper arms and neck when a person exhibits symptoms such as pain and swelling in these regions.
Deep Vein Thrombosis epitomizes a grave medical condition, harboring the potential for consequences that may alter the course of a life. Timely diagnosis through Duplex ultrasound is the keystone of effective intervention and the prevention of complications, such as the ominous pulmonary embolism.
If you, or someone within your sphere of concern, experiences symptoms such as leg pain, swelling, or discomfort of obscure origin, it is imperative to promptly seek medical attention. Contemplating a DVT study can be the critical move that potentially saves a life. In the ever-present shadow of this concealed danger lurking within our veins, vigilance and early detection emerge as the unsung heroes.
“Bringing Experts Together for Unparalleled Vein and Vascular Care”
La Jolla Vein & Vascular (formerly La Jolla Vein Care) is committed to bringing experts together for unparalleled vein and vascular care.
Nisha Bunke, MD, Sarah Lucas, MD, and Amanda Steinberger, MD are specialists who combine their experience and expertise to offer world-class vascular care.
Our accredited center is also a nationally known teaching site and center of excellence.
For more information on treatments and to book a consultation, please give our office a call at 858-550-0330.
For a deeper dive into vein and vascular care, please check out our Youtube Channel at this link, and our website https://ljvascular.com
For more information on varicose veins and eliminating underlying venous insufficiency,
Please follow our social media Instagram Profile and Tik Tok Profile for more fun videos and educational information.
For more blogs and educational content, please check out our clinic’s blog posts!