Varicose Vein Sclerotherapy Treatment: What to Expect
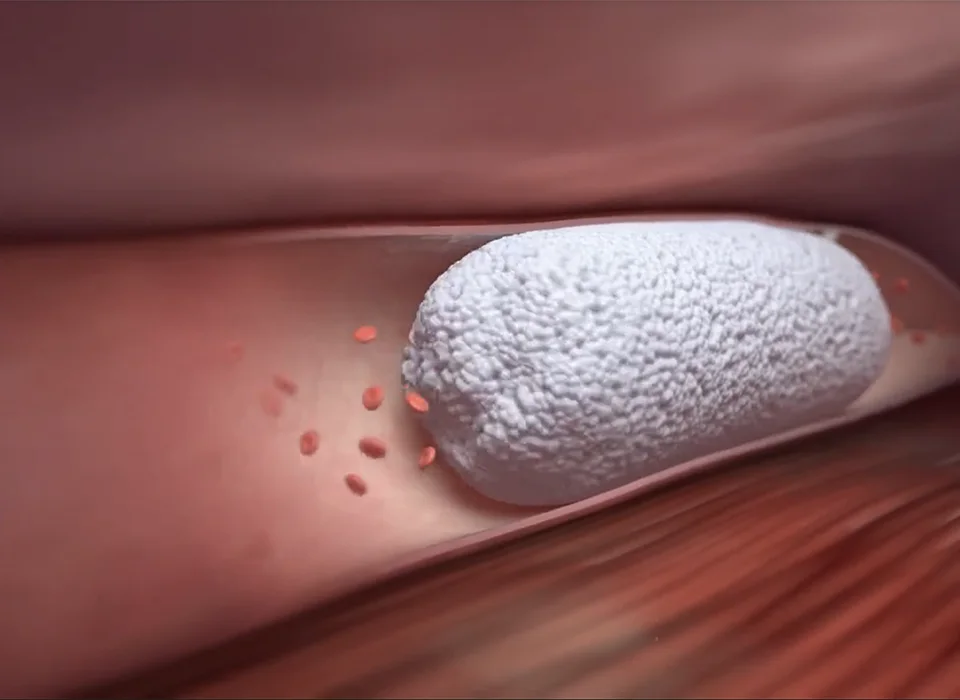
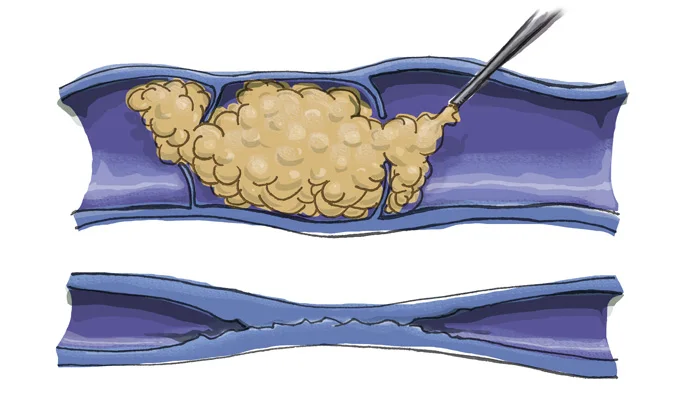
Ultrasound-Guided Foam Sclerotherapy Ultrasound-guided foam sclerotherapy allows your doctor to treat backward flow (or “Venous reflux“) in superficial veins that are not visible to the naked eye but are causing symptoms…