Complications of Untreated Varicose Veins
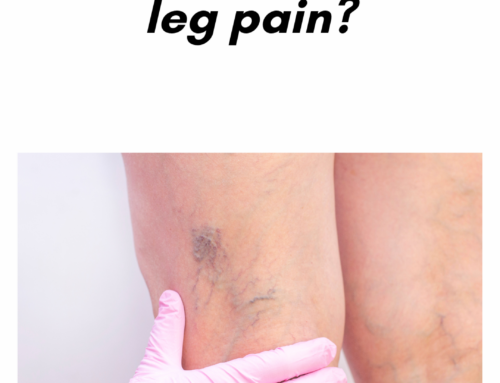
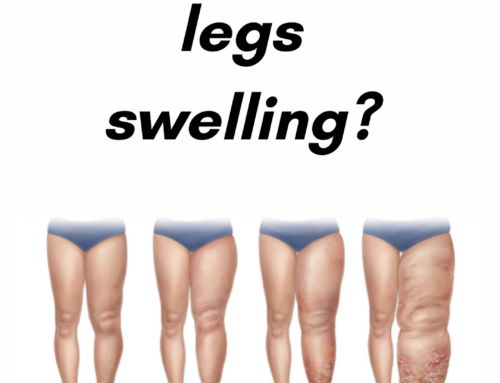
Varicose veins and their underlying cause, venous reflux disease can cause a wide array of symptoms, including leg pain, swelling, aching, heaviness, restless legs, and nocturnal leg cramps.
If left untreated, superficial venous reflux disease can progress to cause skin changes and other complications.
Complications of untreated venous disease include:
1. Superficial Thrombophlebitis (STP)
A thrombophlebitis is swelling and inflammation of a vein caused by a blood clot. There are two main types of thrombophlebitits: deep venous thrombosis (affects deeper, larger veins) and superficial thrombophlebitis (affects veins near the skin surface). This is often referred to as an STP.
The following symptoms are often associated with thrombophlebitis:
Inflammation (swelling) in the part of the body affected
Pain in the part of the body affected
skin redness, warm and tenderness over the vein
Often a ‘hard knot’ or lump can be felt within the vein.
An STP is common complication of varicose veins because blood is pooling and not circulating well. But, it can also indicate an underlying problem with blood clotting. In some cases, there may also be a concurrent blood clot in other veins, such as the deep veins (DVT) which can be serious. For this reason, a duplex ultrasound examination is used to look at the deep veins and other veins not visible to the naked eye for the presence of blood clots.
STP can usually be treated with aspirin or other anti-inflammatory medication to reduce pain and inflammation, compression stockings, and cold/warm packs to also reduce inflammation and discomfort. The discomfort is usually improved within 6 weeks but it can take a few months to resolve.
2. Deep Venous Thrombosis (DVT)
If the blood clot is in a varicose vein near a deep vein or perforator vein, it can extend into the deep system, causing a DVT. For example, a spontaneously thrombosed great saphenous vein, can extend into the common femoral vein and cause a pulmonary embolism (PE). Also, a varicose vein blood clot can extend into a perforator vein and travel to the deep system. It is important to have an ultrasound examination of superficial blood clots to determine a concurrent DVT is present, determine exact location and extent of the superficial clot to make sure it is not near a deep or perforator vein. If it is, a blood thinner may be recommended or serial ultrasounds to monitor the clot may be recommended.
3. Spontaneous Vein Hemorrhage
Untreated varicose veins are at a higher than usual risk of bleeding or spontaneous rupture. Over time, varicose veins become larger, and the vein wall becomes weak and stretched out. These veins, which are already weak are also under high pressure (because of venous reflux, or the ‘backflow’ and pooling of blood in these veins). As a result, the high pressure can cause the veins to spontaneous burst and bleed heavily. Because they are under high pressure, they bleed like an arterial bleed and patients describe the bleeding as ‘blood shooting across the room.’ The varicose veins that are susceptible are veins closest to the surface of the skin
Most patients describe that it occurs during or after a warm shower (warm water causes veins to relax and dilate, allowing more blood to pool within the veins) or during sleep. It is painless and patients report that they notice it because they feel something wet in bed. Patients who are on blood thinners can lose large amounts of blood, especially if it occurs while they are sleeping. Some people have required blood transfusions. The small blue spider veins around the ankle are equally at risk of rupture as are the larger bulging veins.If someone you know has experienced bleeding from their varicose veins, they should be seen by a doctor. Treatment will prevent the veins from bursting again. This is a common condition that we see at La Jolla Vein Care.
4. Venous Leg Ulcer
A leg ulceration is the most severe form of chronic venous insufficiency. This is referred to as a ‘venous leg ulcer.’ Venous leg ulcers make up 70% of all chronic leg wounds. Therefore, the venous leg ulcer is much more common than a diabetic or arterial ulcer. It is caused from long-standing pressure within the leg veins, resulting from 1) venous reflux through faulty valves, 2) a blockage within the deep veins or 3) from the inability to use the calf muscles or a combination. Venous reflux is the most common cause for a venous leg ulcer. The increased pressure within the leg veins (we call this venous hypertension) causes an inflammatory response. Inflammation then causes changes in the skin, usually around the ankles (this is where pressure is the greatest). The inflammatory process will cause the skin around the ankles to become brown or discolored, and eventually the skin will break open. The leg wound can be healed by treating the underlying vein condition.
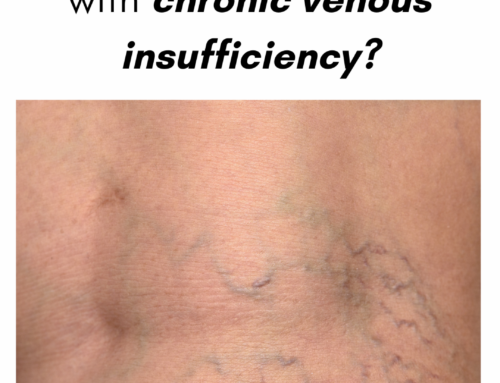
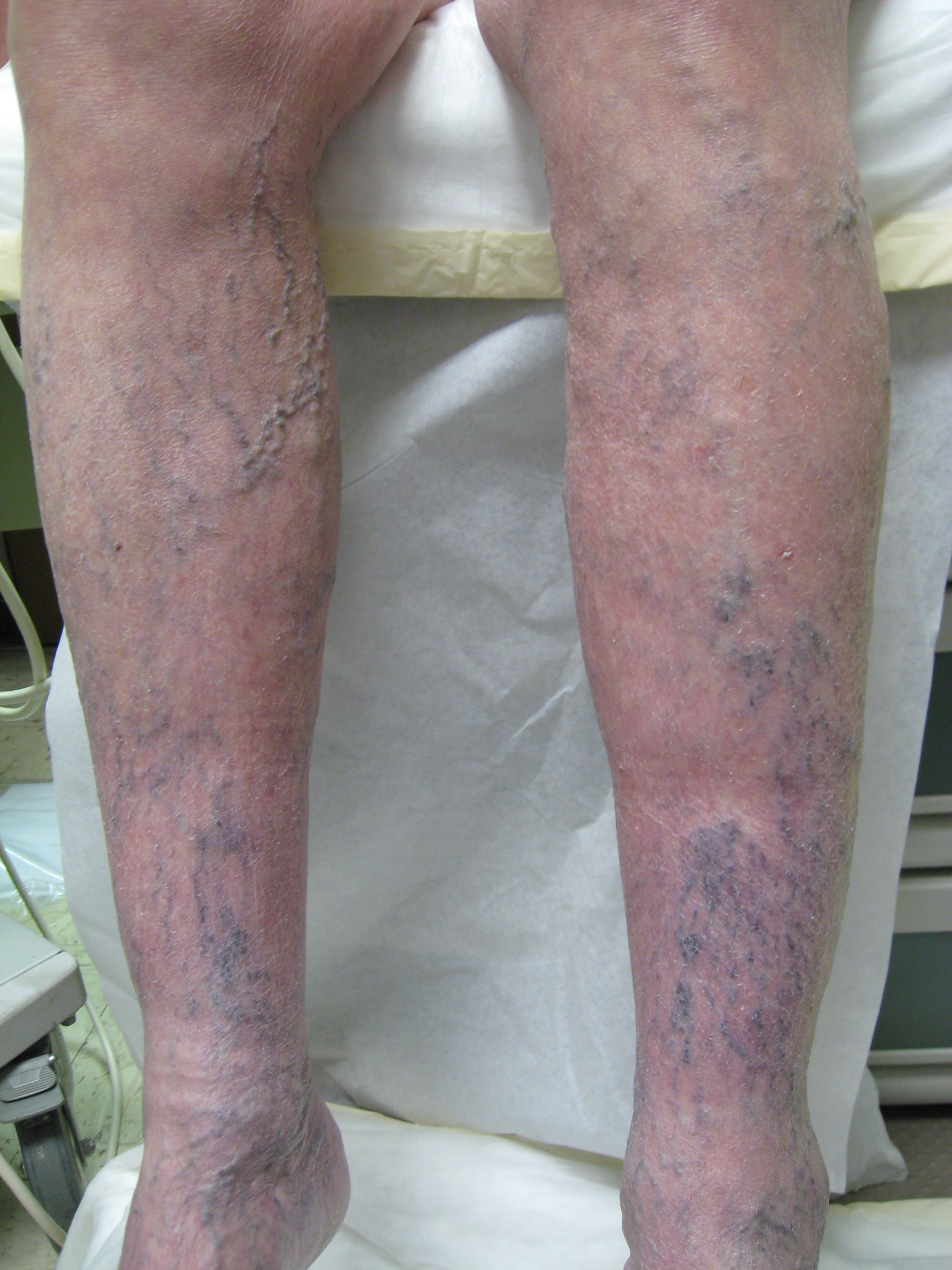
5. Venous stasis and venous eczema
Venous stasis skin changes refers to darkening around the skin. It is associated with itching often, due to inflammation of the skin. It indicates long standing venous disease, called chronic venous insufficiency. Progression can lead to ulceration.
Venous leg ulcers can also be prevented by early intervention with non-invasive procedures. If you have signs of chronic venous insufficiency (such as skin discoloration around the ankles) you should address your underlying vein condition to prevent the skin from breaking open.