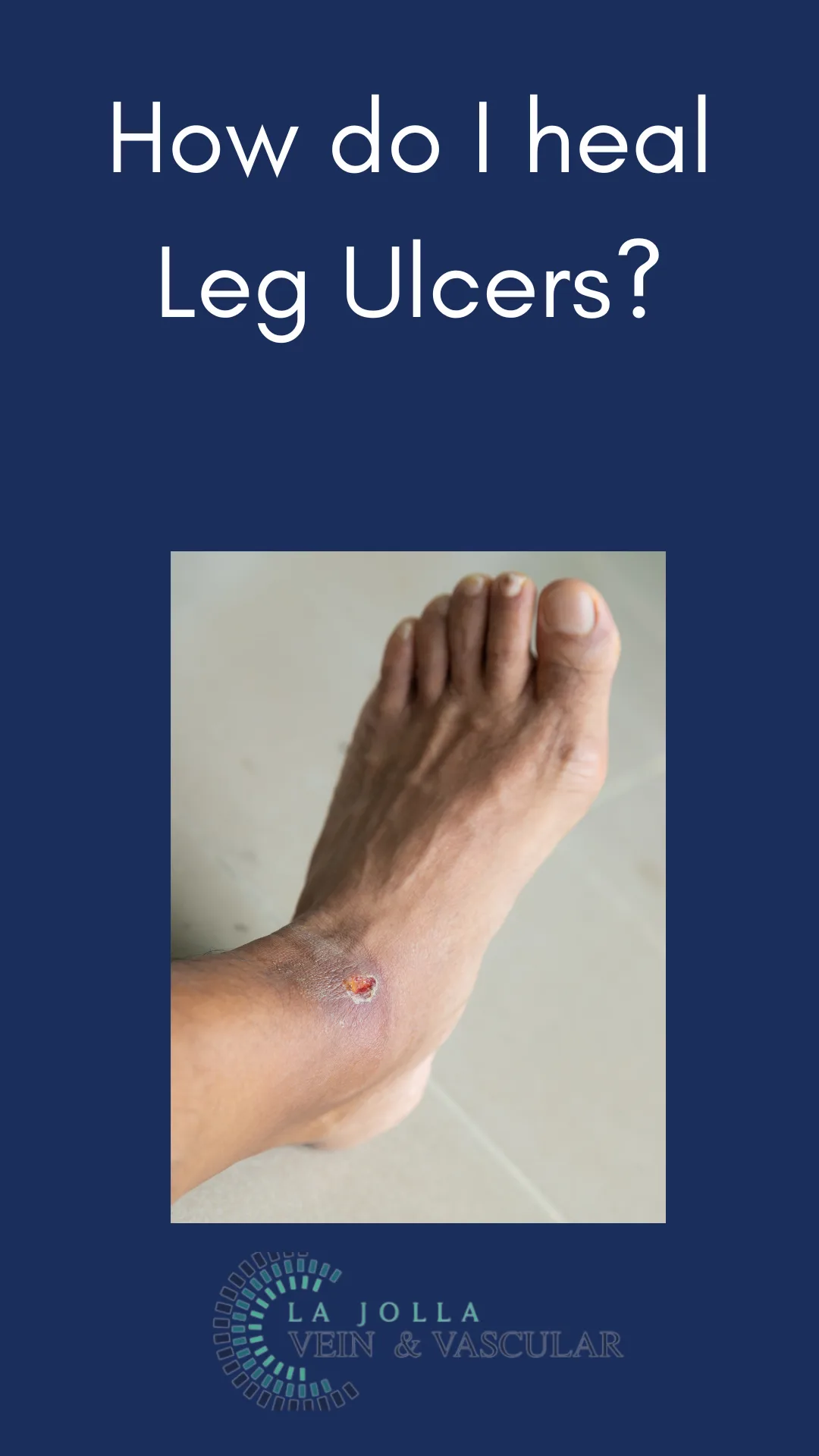
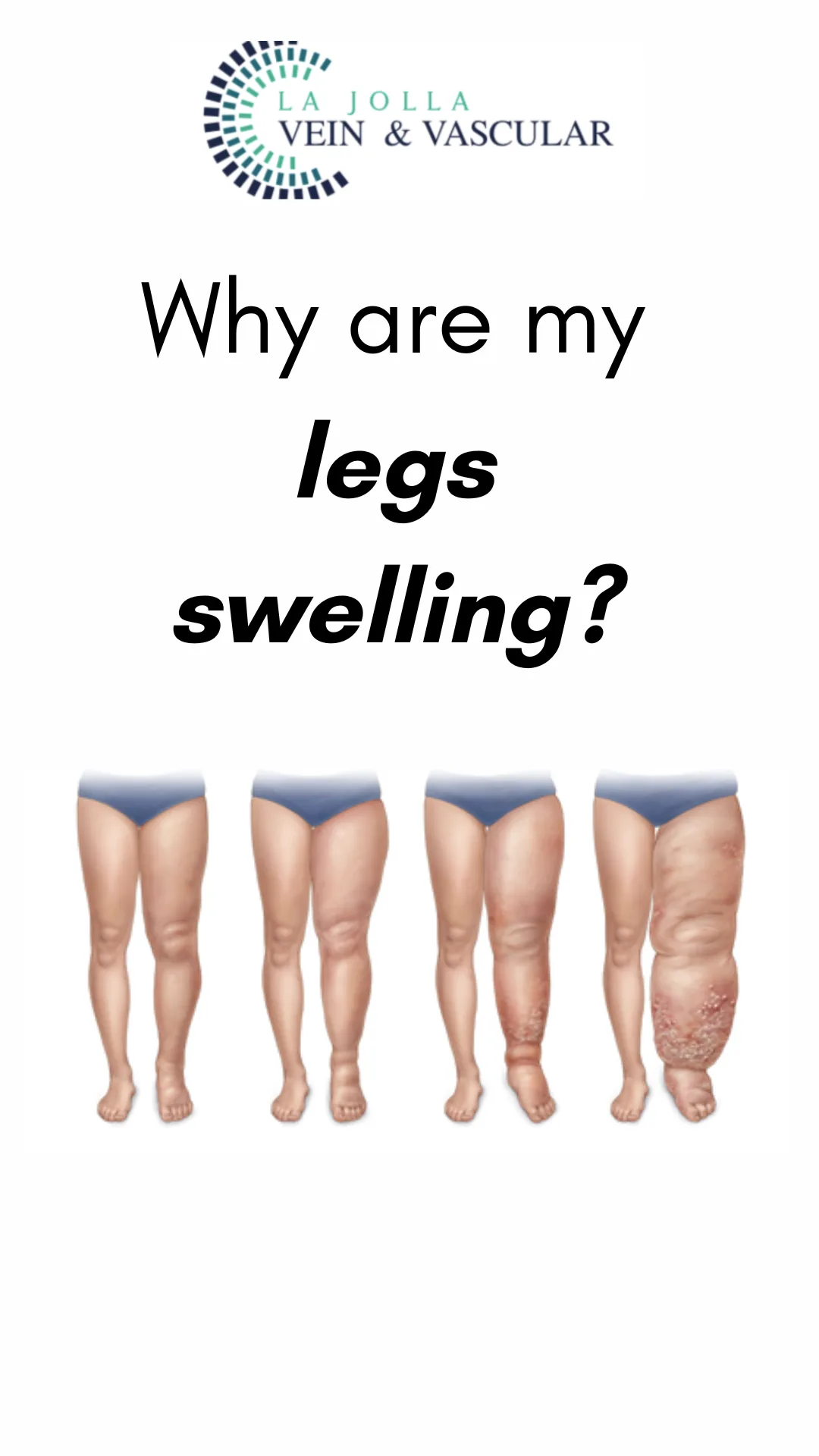
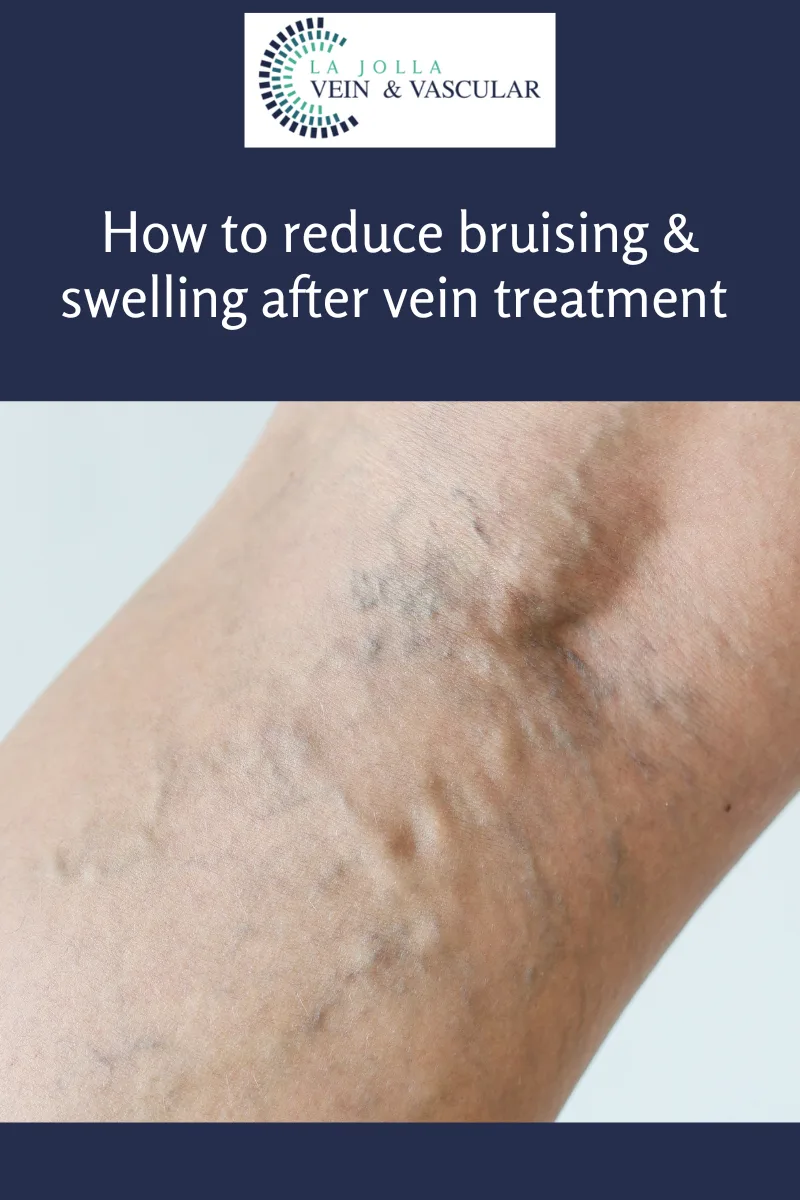
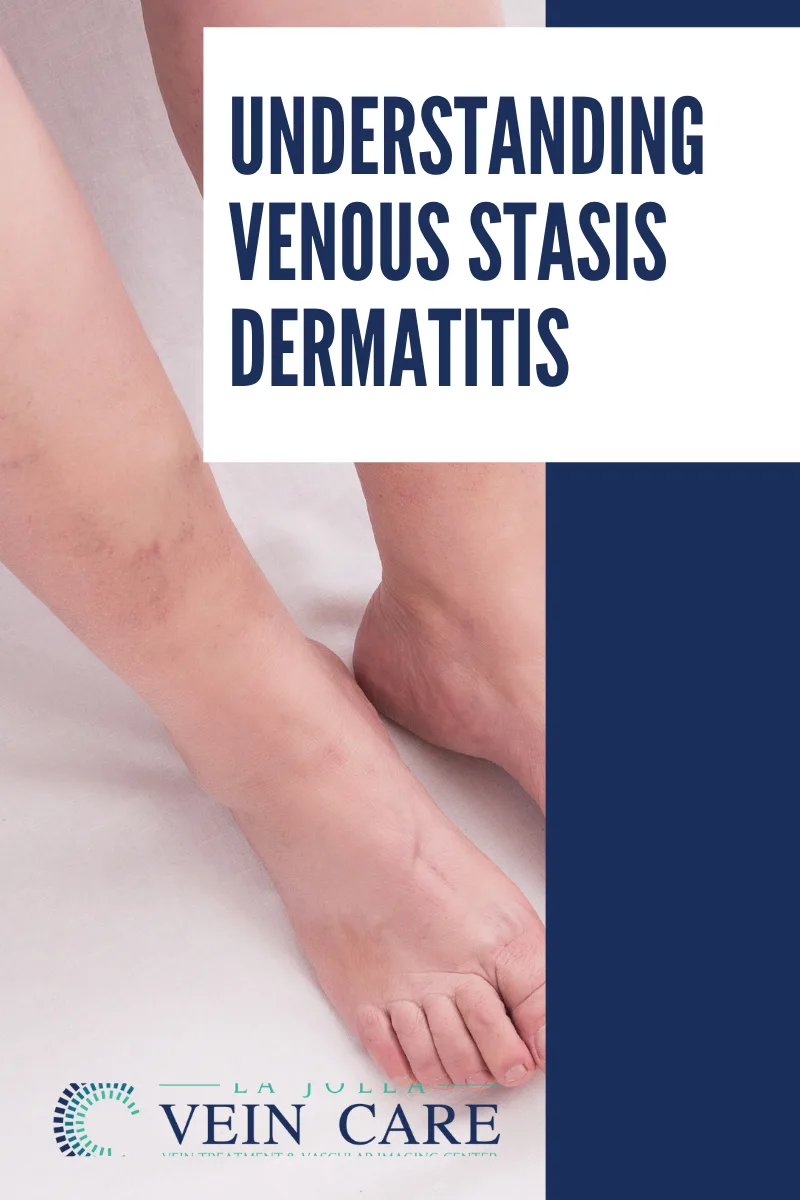
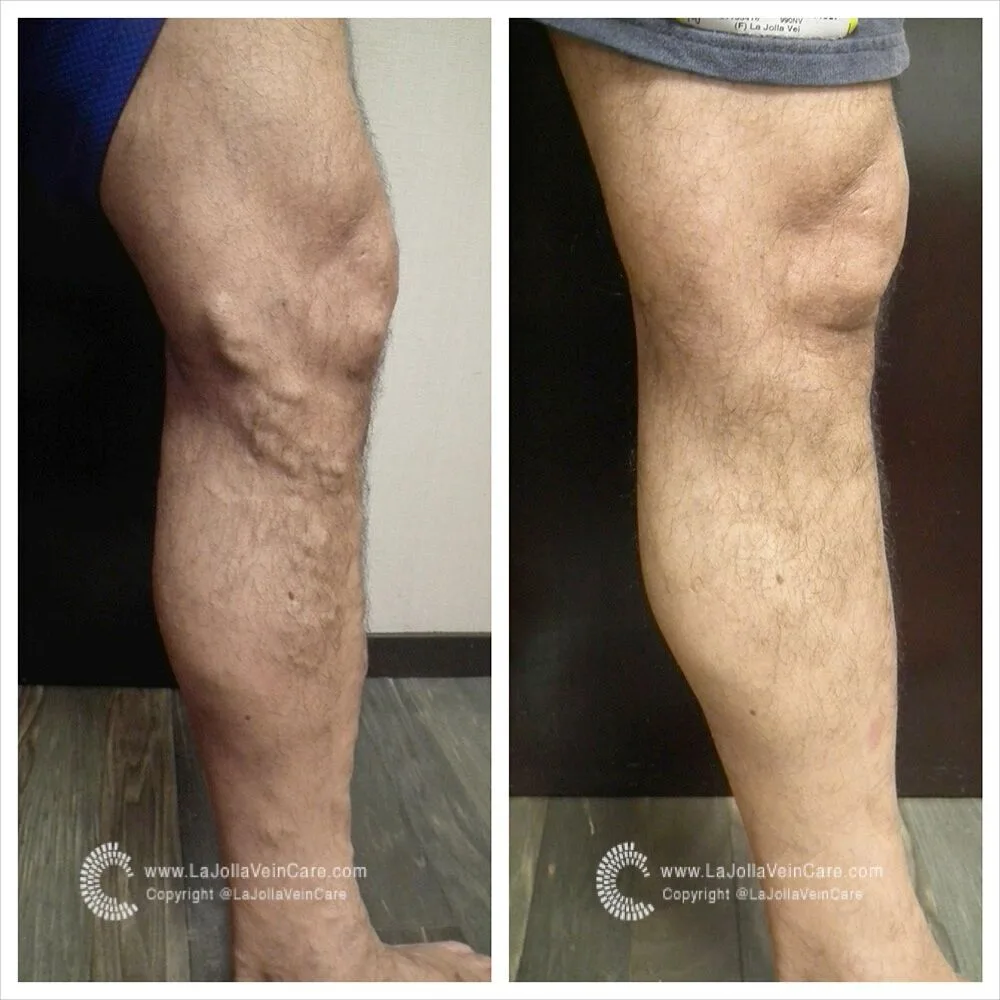
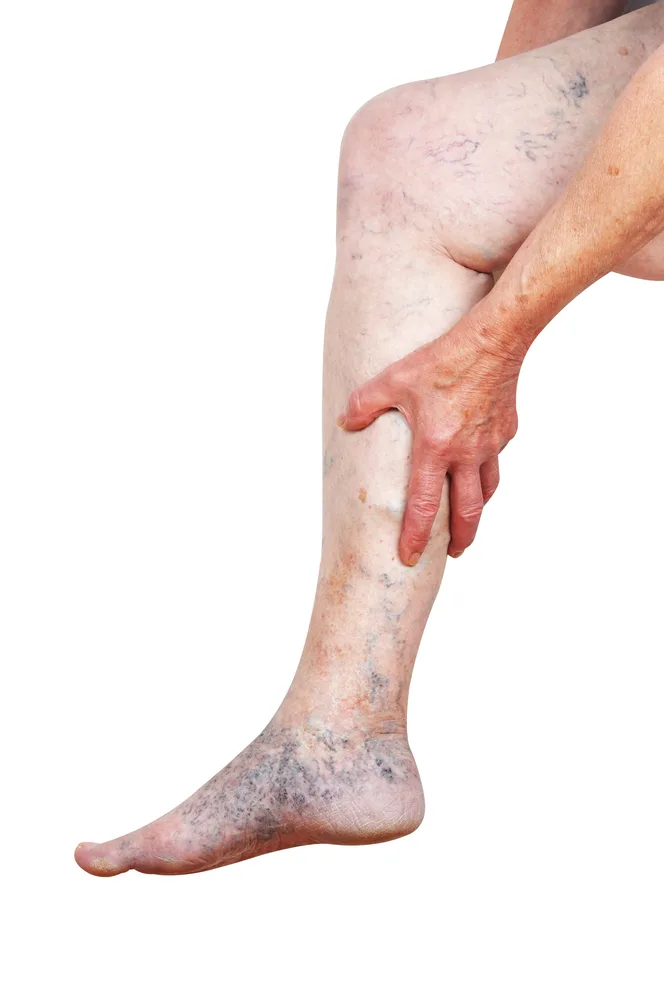
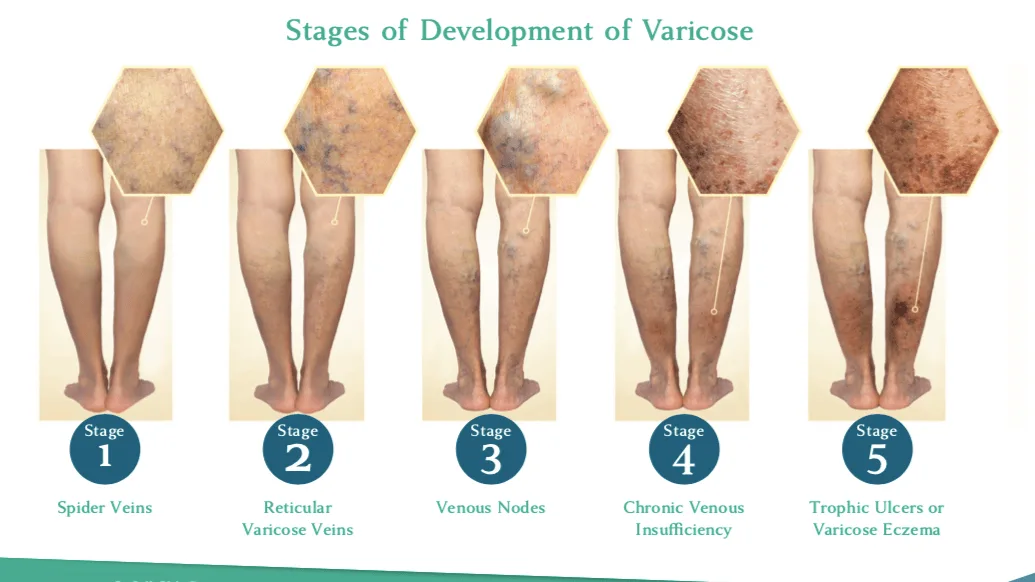
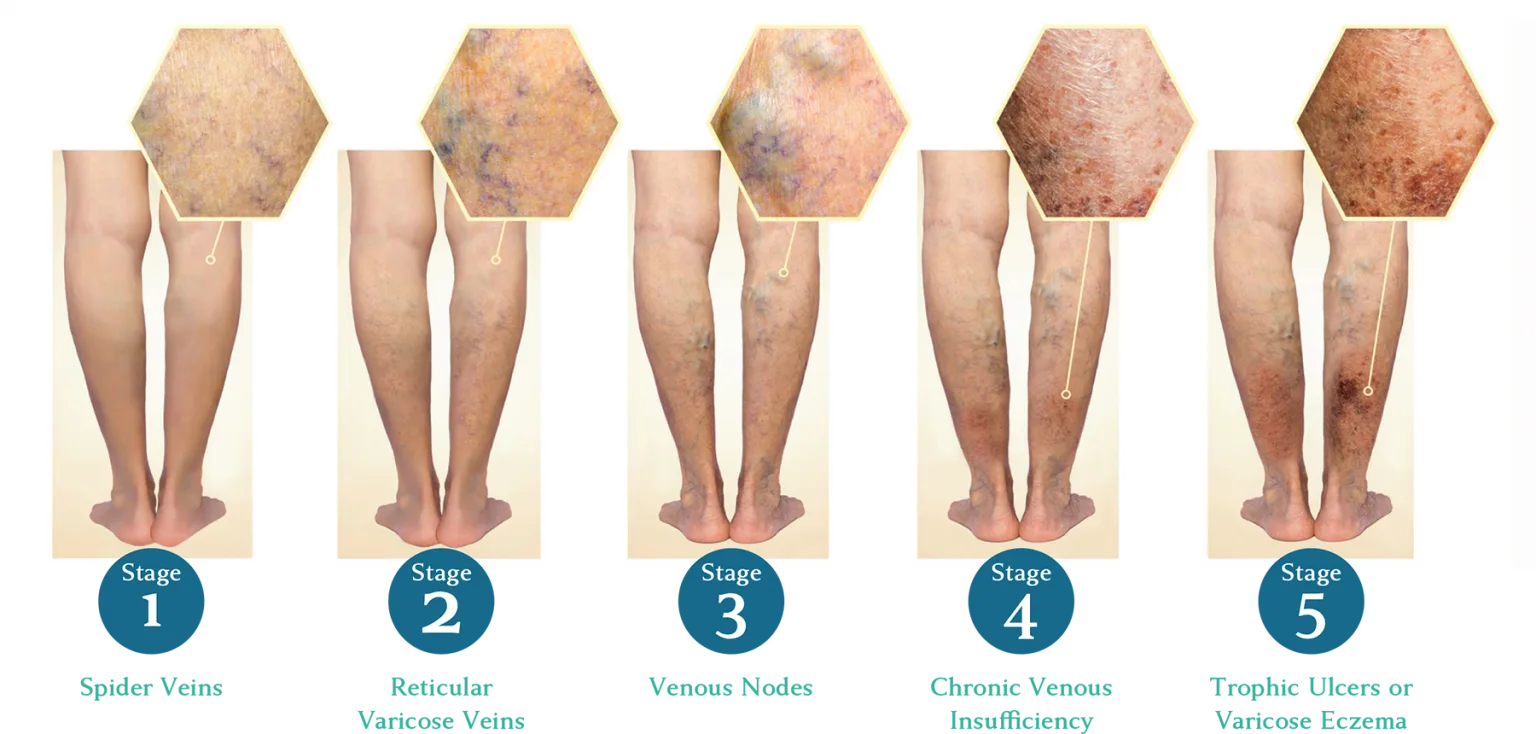
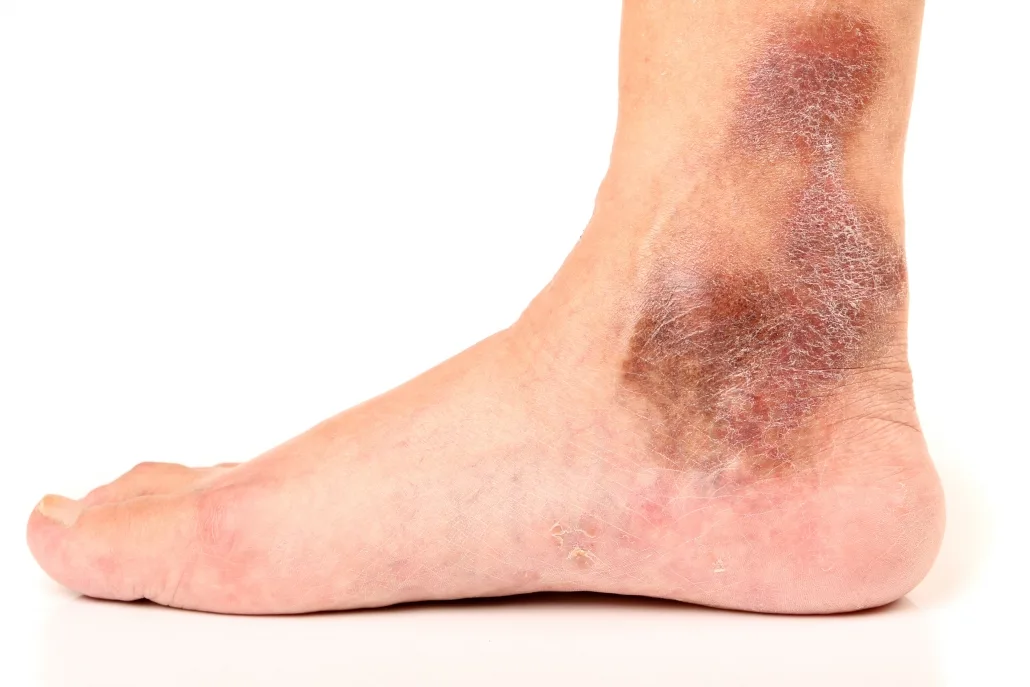
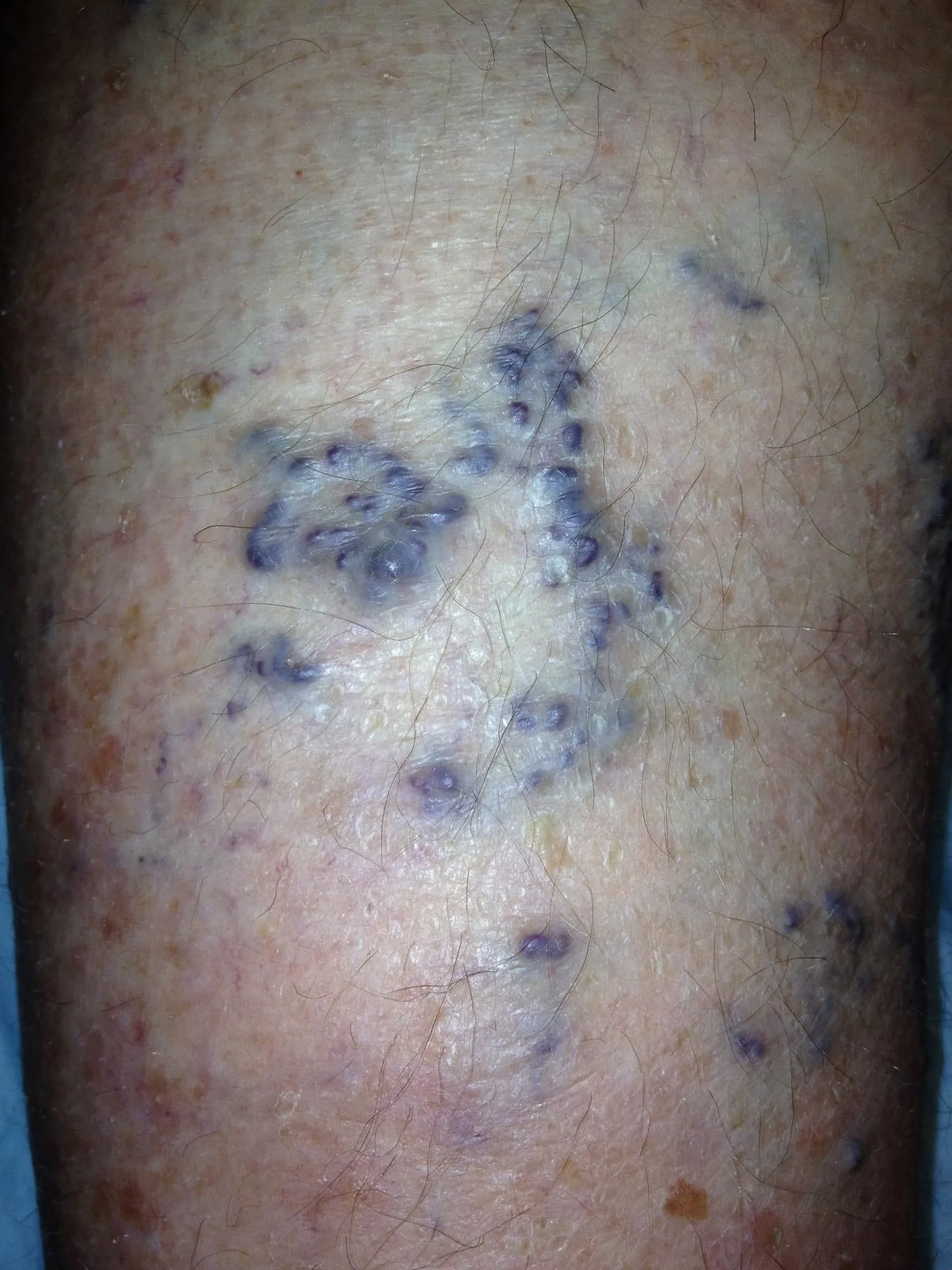
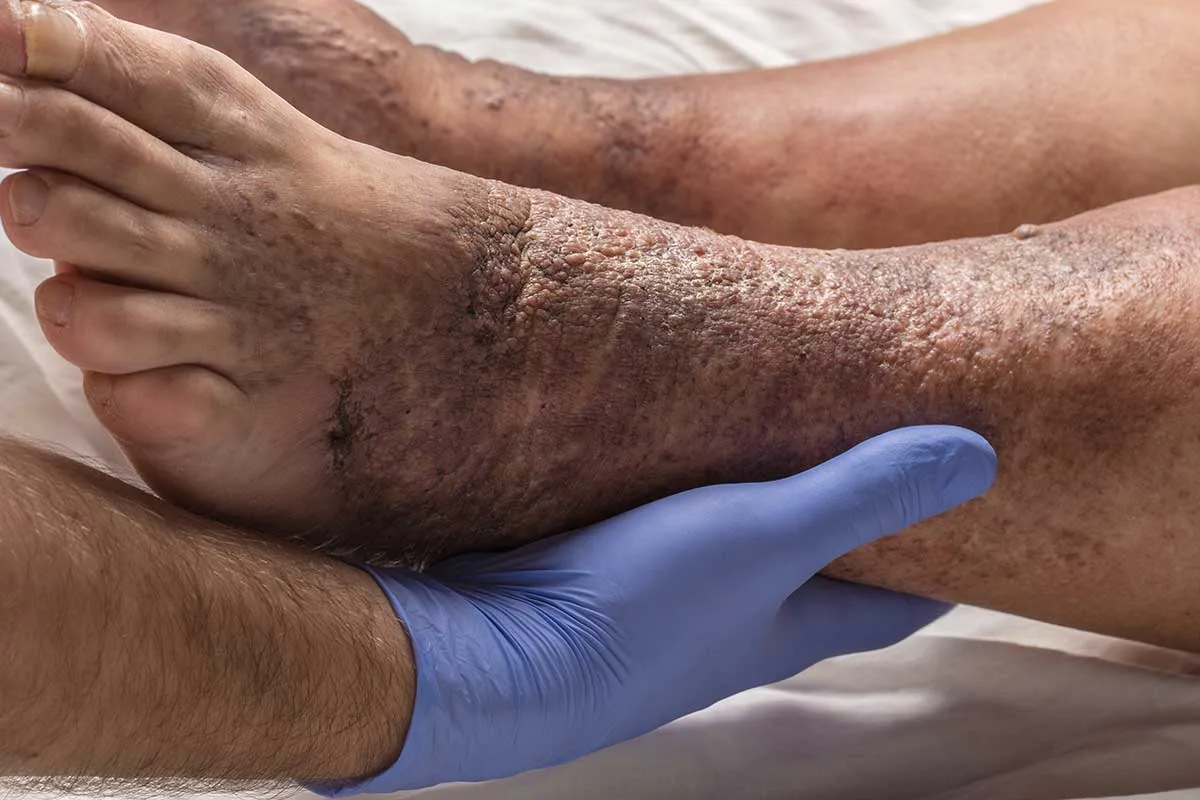
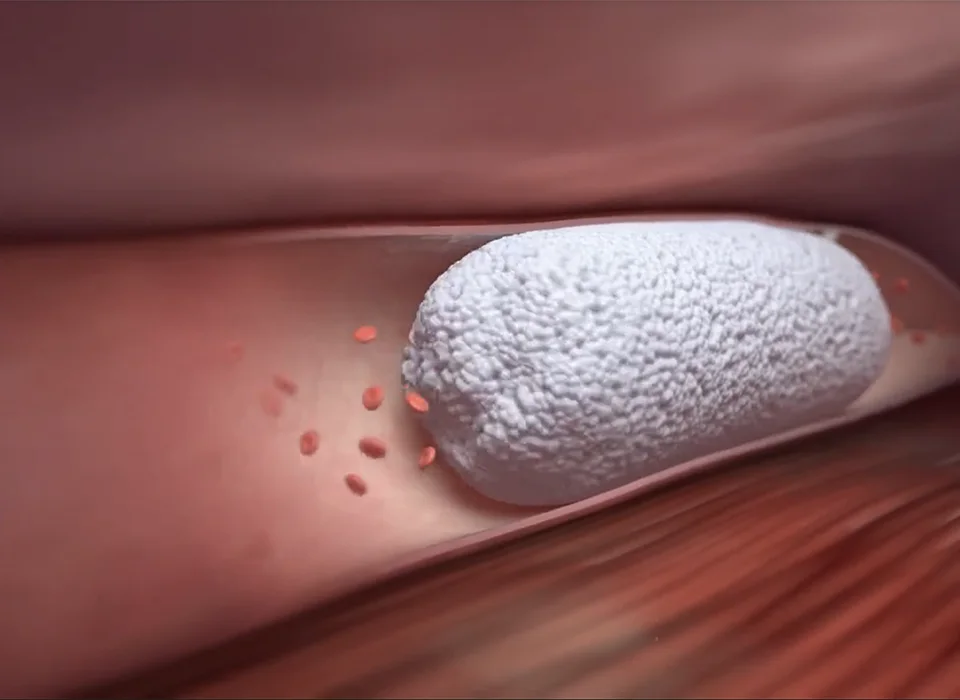
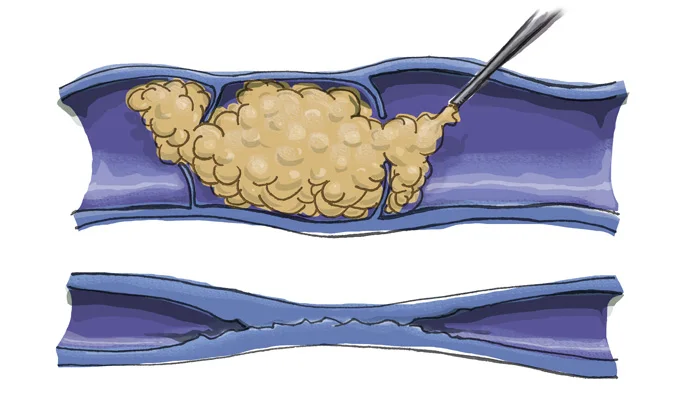
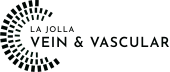Cracking the Code of Chronic Venous Insufficiency: Causes, Symptoms, and Solutions
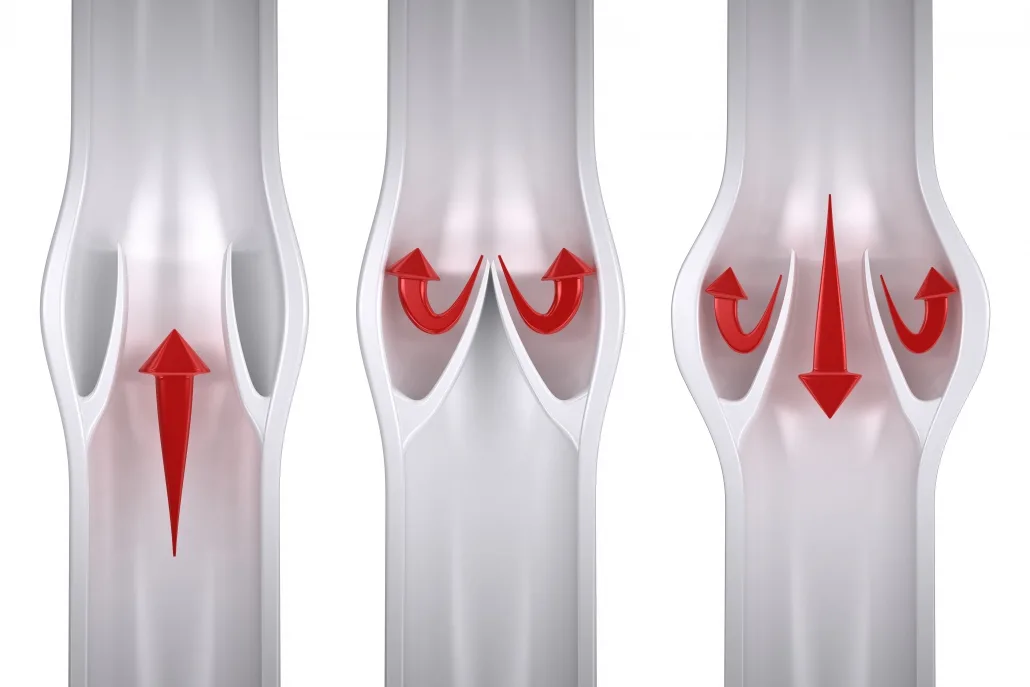
Chronic Venous Insufficiency (CVI) presents itself as a medical condition stemming from untreated venous reflux disease, heralding a plethora of discomforting symptoms. If disregarded, it has the potential to give…