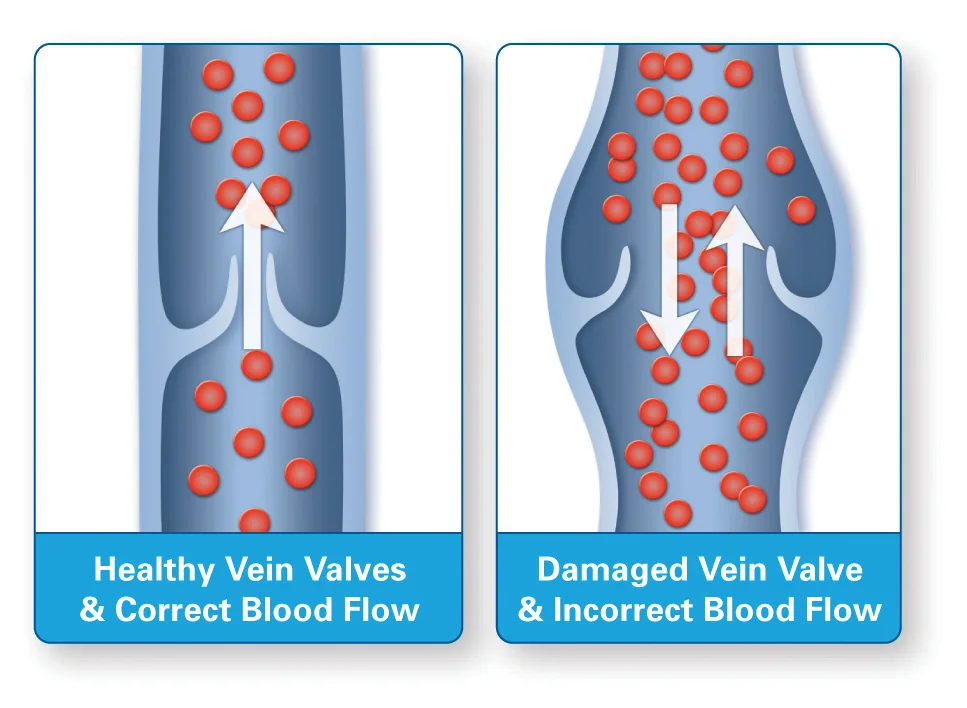
What are Vein Valves?
Vein valves play a critical role in helping blood flow through the veins back to the heart. Like swinging doors, valves open to allow blood to flow toward the heart…


 Find out more about SkinPen®
Find out more about SkinPen®
 Find out more about our Laser Treatments
Find out more about our Laser Treatments